Looking at an embryo under a microscope can reveal how it’s developing, but it doesn’t provide a complete picture of its genetic health. That’s why many individuals and couples undergoing IVF choose to include preimplantation genetic testing (PGT) as part of this process.
PGT offers a closer look at embryos’ genetic makeup, helping identify chromosomal abnormalities or inherited conditions that could affect implantation, pregnancy outcomes, or your child’s health. This information helps your fertility specialist identify the healthiest embryos, allowing you to make informed choices about which ones to transfer and when.
Still, there’s much consider as different types of PGT test for different conditions.
If you're wondering whether PGT is necessary in your case or which type might be appropriate, this guide aims to clarify what PGT involves and how accurate it is. We'll also explore how much it costs and how it may support decision-making throughout the IVF process.
What is preimplantation genetic testing?
Preimplantation genetic testing (PGT) refers to a group of tests done during IVF to analyze your embryos for genetic conditions or chromosomal abnormalities before implantation.
PGT can assess for:
Missing or extra chromosomes (such as Down syndrome) – PGT-A
Single-gene disorders (like cystic fibrosis or sickle cell anemia) – PGT-M
Structural chromosome rearrangements – PGT-SR
In the past, PGT was also known as preimplantation genetic screening (PGS) and preimplantation genetic diagnosis (PGD):
Term | What it refers to |
|---|---|
Preimplantation genetic screening (PGS) | Checks for chromosomal conditions (missing or extra chromosomes) |
Preimplantation genetic diagnosis (PGD) | Checks for specific genetic disorders or inherited conditions |
Today, most clinics use unified terminology under the PGT umbrella.
Bonus: Learn more about preimplantation genetic screening and how it differs from preimplantation genetic diagnosis.
Why do people undergo preimplantation genetic testing?
PGT is beneficial for many different reasons across various scenarios, providing valuable insights that inform embryo selection and reduce the risk of miscarriage or inherited conditions.
Some specific scenarios where it is especially beneficial include:
Maternal age over 35
History of unsuccessful IVF cycles
Being a known carrier of a genetic condition
Past pregnancies with chromosomal abnormalities
In the next few sections, we’ll examine these scenarios more closely.
1. Maternal age over 35
If you’re 35 or older, your doctor might recommend PGT-A as part of your IVF plan. That’s because, with age, the chances of chromosomal abnormalities in embryos increase, especially for conditions like Down syndrome or Turner syndrome.
That doesn’t mean that something will be wrong with your embryos, only that the chances of certain issues slightly increase. PGT-A can help identify embryos with the correct number of chromosomes (referred to as euploidy), which may contribute to a successful implantation.
2. History of unsuccessful IVF cycles
If you’ve already gone through IVF once (or multiple times) without success, your doctor might suggest PGT-A as the next step. Sometimes, even when everything looks fine on paper, embryos may have chromosomal issues that prevent them from implanting or developing.
PGT-A can help pinpoint which embryos are chromosomally normal and give you a clearer picture of which are most likely to lead to a healthy pregnancy.
3. Being a known carrier of a genetic condition
If you or your partner are known carriers of a hereditary condition, like cystic fibrosis, Tay-Sachs, or sickle cell anemia, your doctor might recommend PGT-M.
Being a carrier doesn’t necessarily mean your child will inherit the condition, but it does increase the risk. PGT-M can help identify which embryos are unaffected and give you more information to guide your decisions about which ones to transfer. For many people, it’s a way to reduce uncertainty and feel more in control during a highly demanding IVF process.
Tip 💗
If you want to check whether you or your partner carry certain genetic conditions, try Nucleus Preview. It’s the only carrier screening test that analyzes lifelong health risks and traits beyond rare diseases.

You can take the test at any point in your fertility journey — all reports are easy to interpret and you also have the option to get genetic counseling for further support.
4. Past pregnancies with chromosomal abnormalities
If you have had a past pregnancy affected by a chromosomal condition like Down syndrome or Turner syndrome or have a child with a genetic disorder, your doctor might recommend PGT for future IVF cycles.
PGT can help you better understand which embryos are healthy, so you can make informed choices about which ones to transfer. For many families, it’s a way to feel more confident and supported.
What are the types of embryo preimplantation genetic testing?

Source: Zakir Rushanly
Depending on your personal or family history, your doctor may recommend a specific type of PGT. Some types look for general chromosomal abnormalities, while others focus on inherited conditions or structural changes within the chromosomes.
There are four major types you’ll come across:
Preimplantation genetic testing for aneuploidy (PGT-A)
Preimplantation genetic testing for monogenic conditions (PGT-M)
Preimplantation genetic testing for structural rearrangements (PGT-SR)
Preimplantation genetic testing for polygenic disorders (PGT-P)
Each of these tests screens for different conditions. In the following sections, we’ll break down what each one does.
1. Preimplantation genetic testing for aneuploidy (PGT-A)
PGT-A checks whether your embryos have the right number of chromosomes. Humans typically have 46 chromosomes, but sometimes, an egg or sperm cell doesn’t divide evenly. When this occurs, the embryo may end up with either too many or too few chromosomes, which can impact its ability to implant and develop properly.
PGT-A screens for conditions caused by these chromosomal imbalances, including:
Down syndrome
Turner syndrome
Klinefelter syndrome
Edward syndrome
Patau syndrome
This test can be especially helpful for people over 35 or those who’ve experienced multiple failed IVF cycles since the risk of these abnormalities increases with age and often causes failed implantation.
2. Preimplantation genetic testing for monogenic conditions (PGT-M)
PGT-M is a test designed for people who either have a genetic disorder or are carriers of one. If you or your partner/donor is a known carrier of a single-gene condition, this test can help identify which embryos are affected, so you can avoid transferring one with that specific condition.
PGT-M looks for specific inherited disorders such as:
Cystic fibrosis
Sickle cell anemia
Tay-Sachs disease
Huntington’s disease
BRCA mutations (linked to breast and ovarian cancer)
This test is tailored to your genetic background. Before the embryo can be tested, your clinic would typically have to create a custom probe for your specific condition.
3. Preimplantation genetic testing for structural rearrangement (PGT-SR)
PGT-SR is recommended in situations when one of the biological parents has a known chromosomal structural abnormality, like a translocation or an inversion. This test screens for conditions like:
Reciprocal translocation
Robertsonian translocation
By identifying embryos with normal chromosome structures, PGT-SR may help reduce the risk of miscarriage or failed implantation.
4. Preimplantation genetic testing for polygenic disorders (PGT-P)
PGT-P is one of the most advanced genetic screening options that estimates an embryo’s risk for developing complex diseases influenced by multiple genes. If you have a family history of complex or chronic conditions, your physician may recommend PGT-P testing to proactively identify embryos that have a reduced disease risk.
Some of the conditions the test detects include:
Heart disease
Type 1 and Type 2 diabetes
Certain cancers
Neurodegenerative disorders
Most genetic testing for embryos focuses on identifying rare, single-gene disorders or major chromosomal abnormalities. But many of the conditions that affect quality of life — like those listed above — aren’t caused by a single mutation, which is what makes PGT-P an essential part of preimplantation genetic testing.
When and how is preimplantation genetic testing done?

Source: Gustavo Fring
The PGT process usually involves:
Creating embryos: Your clinic will retrieve your eggs and fertilize them with sperm in the lab to form embryos.
Allowing the embryos to grow: These embryos are then nurtured for 5–7 days until they reach the blastocyst stage when they have sufficient cells for testing.
Biopsy time: At the blastocyst stage, each embryo has a trophectoderm (future placenta) and an inner cell mass (future baby). A few cells are gently taken from the trophectoderm, leaving the inner cell mass untouched.
Freezing the embryos: Once biopsied, the embryos are frozen to keep them safe while you wait for the results.
Testing in the lab: The extracted cells are sent to a lab for analysis, where specialists look for genetic or chromosomal abnormalities, depending on the test you will take.
Many people are concerned that removing cells or freezing the embryo can harm it. The good news is that these procedures are performed with incredible precision, and studies show that they’re generally safe and well-tolerated by embryos.
How long does it take to get PGT results?
The time it takes to receive your PGT results can vary depending on several key factors, but it’s mostly influenced by the type of PGT test you’re doing and the lab or provider handling the analysis. Some tests are relatively fast and follow a standard process, while others are more complex and require time.
Here’s a quick look at the typical waiting times for different types of PGT:
Test | Average turnaround time |
|---|---|
PGT-A | 1–2 weeks |
PGT-SR | 3–5 weeks |
PGT-M | 4–6 weeks |
PGT-P | 2–3 weeks |
Generally, PGT-A has the fastest turnaround time because it follows a fairly standard process. However, for PGT-M, which checks for specific inherited conditions, the lab often needs to create a custom probe tailored to your unique family history. That extra work can extend the timeline.
Bonus: Read this article to get a breakdown of the IVF timeline, including how genetic testing like PGT fits into each stage.
How accurate is preimplantation genetic testing?
It is essential to note that no PGT is 100% accurate. While the technology behind it is advanced and widely trusted, it’s still not completely precise.
There’s a small chance of false positives (where an embryo is flagged as having a condition it doesn’t) or false negatives (where an embryo passes the screening but may still carry an issue). There are also cases where the result comes back inconclusive, and doctors may recommend a repeat biopsy or additional testing to get a clearer picture.
That said, PGT still provides a high level of accuracy overall:
Test | Accuracy |
|---|---|
PGT-A | 98% |
PGT-M | 95–99% |
PGT-SR | 98% |
One gray area that can come up when you undergo PGT-A is mosaicism — when an embryo contains both normal and abnormal cells. Mosaicism can make PGT results more challenging to interpret because the transfer outcome typically depends on the number of abnormal cells and their potential role in the embryo's development. Some mosaic embryos may still lead to healthy pregnancies, while others may not implant at all.
Due to this, your fertility clinic may recommend additional prenatal screening later in pregnancy, like NIPT or amniocentesis, to double-check and confirm results before birth.
Bonus: Discover how accurate PGT-A is in determining the sex of your embryos.
How much does preimplantation genetic testing cost?
There’s no flat fee for PGT. The cost often varies depending on:
The lab your clinic partners with
The type of test you’re doing (PGT-A, PGT-M, or PGT-SR)
The number of tested embryos
Here’s a rough estimate of what people typically pay for different PGT tests:
Test | Cost |
|---|---|
PGT-A | $250–$4,000 |
PGT-M | $2,500–$5,250 |
PGT-SR | From $2,600 |
Overall, PGT-M can be more expensive because the lab has to develop a custom probe specific to the genetic condition you’re testing for. That added step takes more time and more money. If you want to make the process easier and more data-centric, consider getting a carrier screening analysis done by Nucleus, as the results help your doctor identify the conditions for a custom probe.
While PGT is an added cost to an already expensive IVF process, it gives people the peace of mind and insight needed for choosing embryos that may have a better chance of successful implantation or are free from specific genetic risks.
What are the next steps after receiving your PGT results?

Source: Pavel Danilyuk
Once your PGT results are ready, they’re typically sent to your fertility clinic. Your next step will be a consultation with your doctor to discuss the findings in detail. This can be an emotional period, especially if the results show you only have a few viable embryos, or, in some cases, none at all.
It’s completely normal to feel overwhelmed. This is where your support system, both medical and personal, becomes so important. Your doctor will explain what the results imply, discuss possible next steps (which may include another IVF cycle), and help you make informed decisions.
If you do have viable embryos, the next step involves deciding which ones to transfer. Most embryos are frozen after biopsy, so once you’re ready, the selected embryo will be thawed and prepped for transfer — but choosing between embryos alone can be tricky.
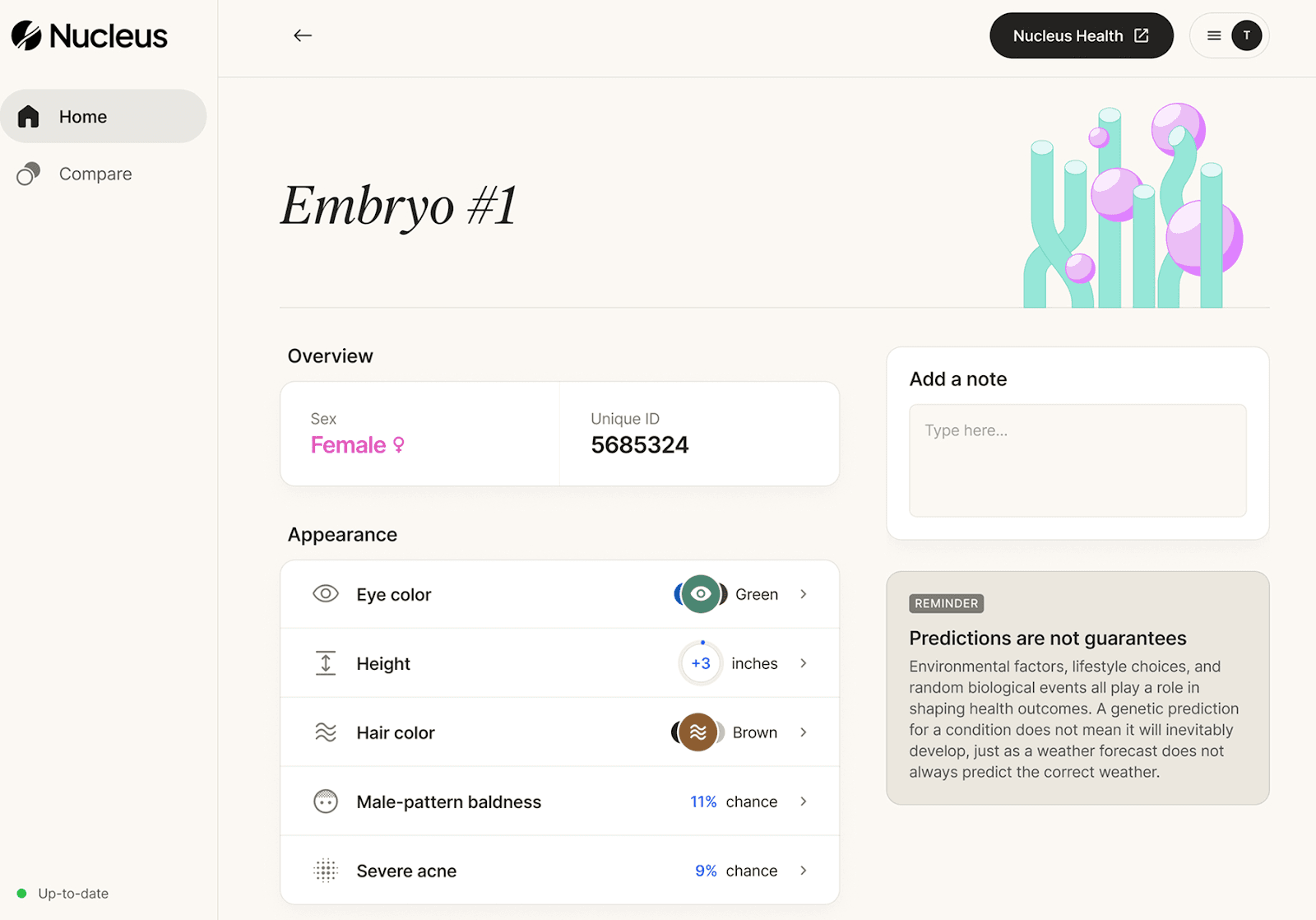
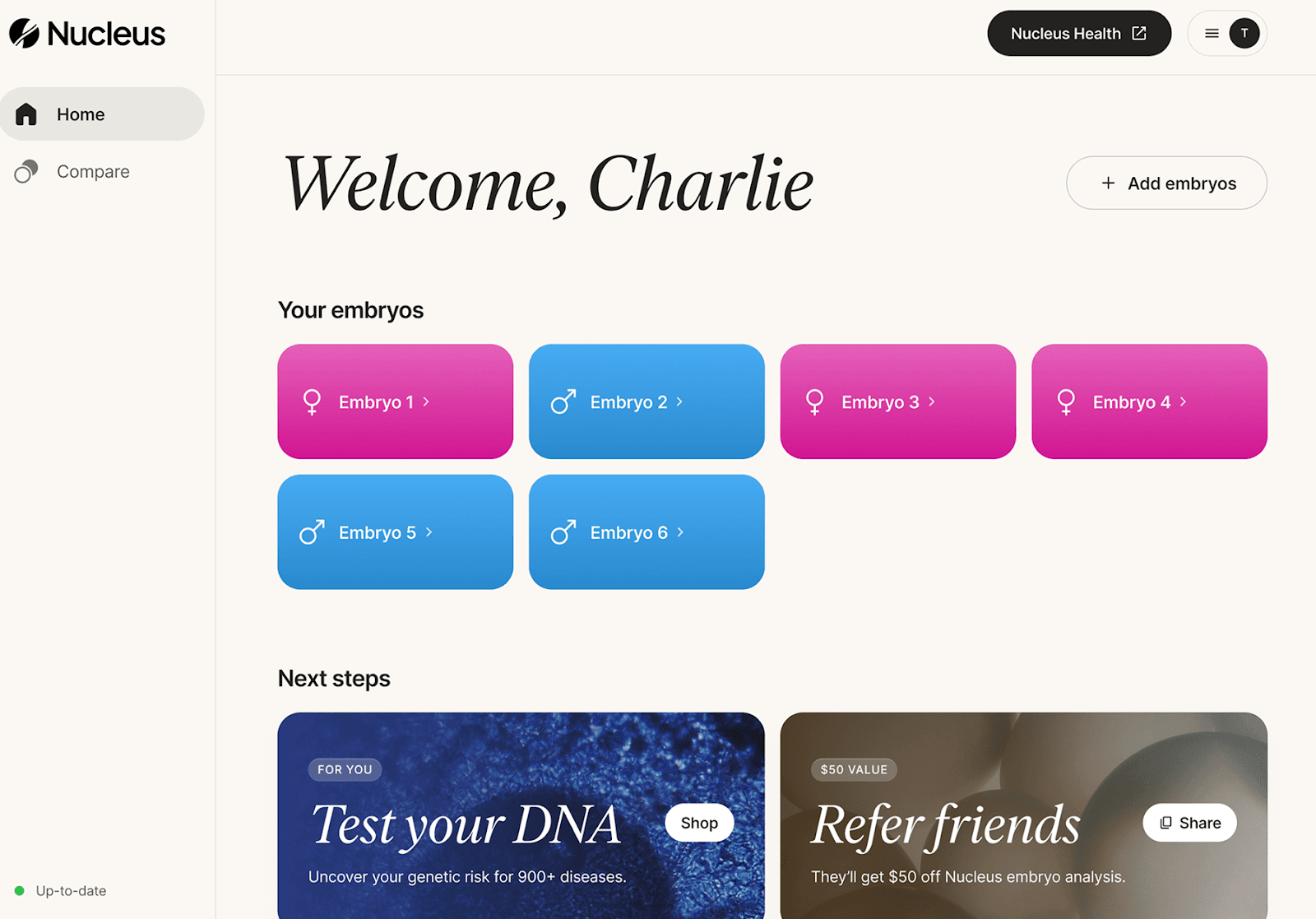
You can also use genetic optimization tools such as Nucleus Embryo alongside PGT testing to access in-depth genetic insights and compare embryos side-by-side. Nucleus Embryo gives you an interactive interface to view the disease risks, physical traits, well-being and mental health of each embryo. The idea is to help you choose what’s best for your family with responsible, science-driven insights.
Learn more about your embryos with Nucleus Embryo
Research shows that many women still view having children as a gamble, and they frequently report a lack of access to the information needed to make informed reproductive decisions.
Nucleus Embryo is about adding clarity and confidence as you make those vital personal choices. There is no one-size-fits-all way when it comes to fertility and family planning, which is why Nucleus built a platform that lays out all scientifically credible information for parents and helps them make their choices with care, transparency, and responsibility.
When choosing which embryo to transfer, Nucleus Embryo can help you explore your embryos more holistically.
Once you have your PGT results, sign up for Nucleus Embryo to get deeper insights on each embryo’s genetic makeup. You can get information on how the embryos fare in terms of developing potential:
Health conditions: Heart disease, cancer risk, ADHD, depression, and dozens of other hereditary disorders
Physical traits: Eye color, height, hair color, male-pattern baldness
Well-being: Markers for intelligence, mental health risks, and more
The best part is that Nucleus is designed to be used by parents, not scientists and physicians. You get to sort, compare, and select embryos in a clean, easy-to-navigate interface — at your own pace.
You may also like…
Featured image source: Gustavo Fring


















